
Dandruff: a mini-guide
13/09/2023
Folliculitis: focus
20/09/2023Indice
Anonychia: absence of the nail plate
Anonychia is the absence of the nail and can be congenital or acquired. Congenital cases of anonychia are, however, rare and are most often accompanied by other developmental disorders. On the other hand, acquired anonychia can be the result of inflammatory diseases such as lichen or psoriasis.
Anonychia can be total or partial, depending on whether some or all laminae are missing.


Chromonychia: lamina color change
The change in lamina colour can be of external origin, such as contact with oxidising substances.
For example oxidation of the lamina by potassium permanganate.
Or from internal causes.
It can also be the result of internal factors, with the main endogenous causes of chromonychia being disease or the use of certain drugs.
When chromonychia is the result of disease, it is usually due to the absorption of toxic substances from within the work environment.
Instead, when the cause is medication, it is often due to certain drugs such as antibiotics or chemotherapeutics that can cause nail discoloration.
Leuconichia and melanonychia are considered separately among chromonychias.

Leukonychia: white marks on the lamina
The white marks characteristic of leukonychia may appear as dots, horizontal or vertical lines, or may turn the entire lamina white.
There are both congenital forms of leukonychia and those caused either by disease or external factors.
The most common external cause is trauma induced by extreme pedicures or through the wear of unsuitable shoes.
Below is an example of horizontal leukonychia striata (Mees’ lines):

Leukonychia totalis
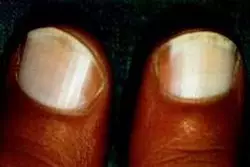
In addition to leukonychia, other noticeable color changes to the nail include:
- blue nails, usually resulting from drugs such as tetracycline or chloroquine;
- green nails, usually resulting from a pseudomonas colonization;
- yellow nails, usually resulting from hyperthyroidism or medications.

Melanonychia: black staining of the lamina
Black coloration of the nails can appear for many reasons:
- from medication (e.g. chemotherapy)
- from disease (e.g. renal failure)
- from melanin (e.g. nevus, melanoma)
- from bleeding (e.g. trauma)


Onychodystrophy: nail growth disorder due to nutrient deficiency
Onychodystrophy is mainly caused by a lack of blood supply to the germinal matrix. It can also be linked to insufficiently oxygenated blood supply to the area, or a blood supply deficient in nutritional factors.
Blood flow is affected when blood vessels become occluded, for example as a result of trauma or because of diabetic/atherosclerotic angiopathy. Another cause is when blood pressure drops due to cardiological problems or when the lungs fail to properly oxygenate the blood. In other cases, the blood supply is there, but it is nutritionally lacking. This can occur due to illnesses such as liver disease, or as a result of chemotherapy, malabsorption, or dietary deficiencies. In any case, the most frequent cause of onychodystrophy is senescence.
A summary of the other most common causes are:
- Trauma
- Cardiovascular disease
- Diabetes
- Respiratory failure
- Cirrhotic hepatopathy
- Chemotherapy
- Senescence

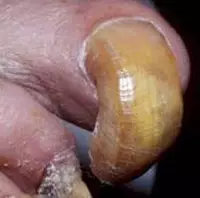
Onychogryphosis: ram’s horn nail
Onychogryphosis occurs when the nail plate thickens to the point the patient can no longer cut it, which causes it to continue growing until it begins to curve to take on the appearance of a claw.
Onychogryphosis usually prevents normal walking and must be corrected surgically.
Onychogryphosis is sometimes linked to onychodystrophy, but can appear independently due to altered neuronal stimuli to the germinal matrix.
In other cases, onychogryphosis can be triggered by trauma obtained through sports such as tennis, volleyball and basketball.
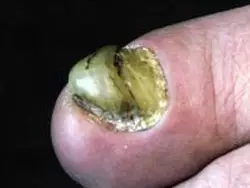
Pachyonychia: the thickening of the nail plate
Pachyonychia causes the nail plate, and particularly that of the big toe, to thicken when the germinal matrix is hyperproliferative. This can occur in cases of psoriasis, or if the patient has nutritional deficiencies as can often occur in senescence.
A special case is pachyonychia post-avulsion of the lamina, whereby lamina avulsion causes the distal phalanx to tip upward.
As the lamina grows, it bumps against the phalangeal soft parts and can no longer slide horizontally so it grows vertically creating pachyonychia.
senile pachyonychia

psoriasis pachyonychia

post-avulsion pachyonychia
Onycholysis: detachment of the nail plate and separation of the lamellae
Onycholysis describes either when the lamina detaches from the nail bed, or when individual lamellae do not adhere to each other.
It is the most characteristic sign of nail psoriasis.
It may also occur from repeated trauma (sports, footwear, etc.) and sometimes as a side effect in the use of certain medications.
- Psoriasis
- Trauma
- Medications
Onychocryptosis: ingrown toenail
Onychocryptosis, commonly referred to as ingrown toenails, is one of the most common pathological occurrences and primarily affects the first toe.
Ingrown toenails can often be accompanied by the reactive granulomas due to the irritation that the lamina causes to the dermis.

Paronychia : Inflammation or infection of the perionichia
Paronychia is the inflammation or infection of the tissues surrounding the nail. It is most often infectious and is preceded by inflammation following, for example, trauma or contact with irritants.
Infectious paronychia can be the result of:
- Staphylococcus
- Dermatophyte
- Candida
- Herpes simplex
paronychia from herpes simplex

paronychia from candida

Onychomycosis is an uncommon occurrence that is usually associated with a pre-existing alteration of the nail plate following conditions such as psoriasis, dystrophy, or trauma.
The fungal infection usually parasitizes the nail bed, but can also attack the lamina itself.
Onychomycosis: parasitization of the nail by mycetes
Supralaminar parasitization

Intralaminar parasitization

Sublaminar parasitization

The fungi that cause onychomycosis belong to the genus:
- Keratinophilic dermatophytes
- Yeasts
- Molds










