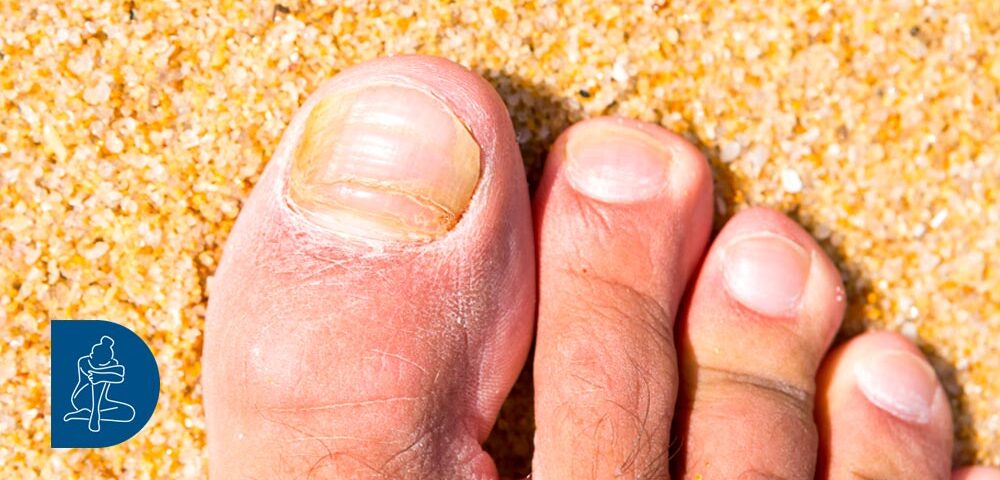
Plantar dyshidrosis: treatment according to DermaClub
21/09/2023
Athlete’s foot: pharmacological treatments and alternative remedies
21/09/2023Toenail fungus is a rare condition, at least as long as the nail plates remain intact and undamaged by other diseases or trauma. However, diagnoses of toenail fungus are as common as they are incorrect, with the unfortunate consequence that many people undergo lengthy and costly treatments that have no effect.
The reasons for these misdiagnoses lie in a poor understanding of the clinical presentation of nail fungal infections and in the fact that certain species of fungi can be found in toenails which, however, do not cause any symptoms and are not the cause of the nail condition; consequently, they do not respond to treatment with antifungals.
Indice
Onychomycosis describes a nail that has been invaded by fungal elements
Onychomycosis is the general term used to describe a fungal infection of the nail.
Fungal organisms have a complex and as yet not definitive classification; in dermatology, this classification comprises three groups: dermatophytes, yeasts and moulds.
Dermatophytes are fungi known as keratinophilic fungi because they feed on keratin, which is the main protein in the stratum corneum, hair and nails.

This means that this group of fungi can affect only the skin surface and its appendages, but not other parts of the body. Skin and appendage infections caused by dermatophytes, known as ringworm, are mainly attributable to the species Trichophyton and Mentagrophytes.
Moulds, which cause serious systemic infections in immunocompromised individuals, can also be found on the skin without, however, causing disease. Among moulds, Scopulariopsis brevicaulis, Fusarium sp. and Aspergillus sp. are the most frequently isolated.
Yeasts, represented mainly by Candida species, are single-celled microorganisms like bacteria and may be found incidentally on the skin, where they do not cause disease; however, disease may arise in moist environments such as the mouth (thrush) and the vagina (vaginal candidiasis).
Various forms of onychomycosis
Lateral distal subungual onychomycosis
It’s the most frequent form of toenail fungus, lateral distal subungual onychomycosis, it arises from a fungal infection between the toes, which then spreads to the foot and then to the nail bed. Inflammation is present.
Proximal subungual onychomycosis (PSO)
It is the rarest form of onychomycosis, in which colonization of the nail matrix occurs through the proximal fold and is followed by invasion of the proximal part of the lamina.
White superficial onychomycosis (WSO)
A rare form of onychomycosis, WSO is caused by the direct invasion of the nail plate’s surface. The proximal portion appears white and the surface of the lamina is intact. WSO is present in about 90% of immunocompromised patients.
Endonyx (EO)
It is a variant of distal lateral subungual onychomycosis.
The infection spreads directly from the skin to the nail plate.
While onychomycosis may appear common, it is actually a very rare occurrence and is often confused for other nail conditions at the point of diagnosis.

Why is onychomycosis so often misdiagnosed?
The main reason for misdiagnosis and, therefore, mistreatment lies in confusing onychomycosis with other, much more common nail diseases such as nail psoriasis or onychodystrophy. In addition, medical terminology needs to be updated to allow for more accurate diagnosis.
If yeast or mold is found on the nail, does it automatically mean onychomycosis is present?
The answer is NO. Yeast or mold can only be found on the nail plate once it has already been damaged or disrupted by another pathology such as psoriasis or onychodystrophy. They are not the original cause of nail damage, but are the original pathology that has allowed the molds or yeasts to establish themselves. Cases of yeast or mold on the nail are, therefore, a contamination, not a parasitism of the nail. In terms of treatment, if the contaminated nail is treated with local or systemic antifungals, the yeast or mold may well be eliminated but the nail and the damage remain. This treatment failure is widespread in cases of yeast and mold on the nail.
Keratinophilic Dermatophytes = Onychomycosis
It is therefore appropriate to speak of Onychomycosis only when keratinophilic dermatophytes are involved, as these break down keratin, damaging or destroying the nail. In these cases – which are, however, very rare – it makes sense to use a topical or systemic antifungal agent, bearing in mind, however, that dermatophytes are not very sensitive to common antifungals such as imidazoles and allylamines.
Even in cases of onychomycosis caused by dermatophytes, it is worth noting that the fungal infection may have occurred due to pre-existing structural damage to the nail plate caused by another condition; consequently, even after prolonged pharmacological treatment to eliminate the dermatophytes, the nail plate may not return to its original state.
Conditions that create the confusion with Onychomycosis
Nail psoriasis
Psoriasis of the nails, on the other hand, is a very common condition. It can affect both the nail plates of the hands and the feet.
An important clinical sign to look for in the diagnosis of psoriatic nail disease is the so-called ‘nail separation’. The presence of an intact nail plate situated between two or more damaged plates should lead to a diagnosis of psoriatic onychopathy rather than onychomycosis, as there is no reason why a fungus would skip a nail rather than infect it.
If signs of psoriasis are also present elsewhere on the body, the diagnosis of psoriatic onychopathy becomes automatic.
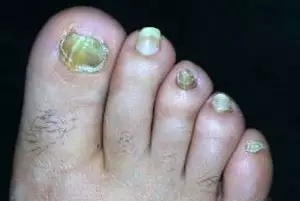
Onychodystrophy
Onychodystrophy is the second most common condition mistaken for onychomycosis.
This refers to nails that, due to vascular problems (ageing, diabetes, vascular disease, nutritional deficiencies, chemotherapy, trauma, etc.), are no longer able to grow healthily. The nail plates appear opaque, ridged, sometimes detached from the nail bed, growing vertically rather than horizontally, and so on. In addition to these growth defects, there may also be an infestation by moulds or yeasts which, taking advantage of the nail plate’s compromised state, penetrate the nail.
This is not true onychomycosis but fungal contamination on top of nail dystrophy.
It is easy to see that the problem in these cases is not the fungal infection but the dystrophy, and consequently treating the parasitic fungus is of minimal value. Indeed, even if the fungus is eradicated, the nail remains pathological and unchanged due to the dystrophy.
Treatment considerations
Treating onychomycosis is always difficult, and before embarking on any treatment, it is advisable to weigh up the costs and benefits of doing so.
The main points to consider are: the slow growth of the nail plate, the toxicity of systemic antifungal drugs, the limited effectiveness of topical antifungals, and the frequency of recurrence following treatment.
Confusing treatment options
Recently, laser or photodynamic therapy have become popular to treat onychomycosis, however these treatments have no scientific basis in the cure of the condition and should, therefore, be dismissed.
Dermaclub recommends
The most sensible podiatric treatment involves repeated filing of the infected nail plates, alternating with a period of daily application of sulphosalicylic acid cream (Onicosana), in addition to addressing any behavioural issues on the part of the patient or structural foot defects that may be contributing factors to the fungal nail infection.